Six things you should know about eczema

Posted on
I’ve always been lucky in the skin stakes – no acne, no warts, and no eczema.
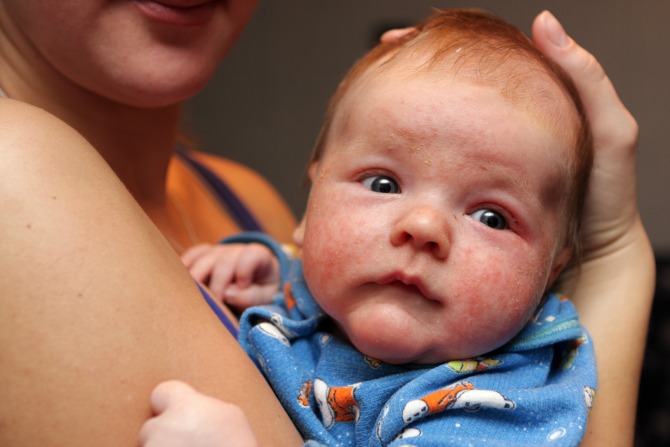
So I was surprised when both my girls developed the latter condition in the first few months of their lives. Sophia, in particular, suffered terribly with red, raw patches on her face and under her ears that were only cured by steroid cream.
It’s an increasingly common story. In the last 50 years, more and more children – and adults, too — are suffering from eczema. At least three of the kids in my Mothers Group had eczema at some point, and we lived collectively through a dietary regime free of eggs, diary and wheat.
So, why is eczema on the rise? And what can we do to manage the condition? I spoke to Luke Clews at Healthy Skin Solutions in Kingston to find out.
1. First things first: what is eczema?
Luke: Eczema (also known as atopic dermatitis) is a chronic inflammatory skin condition with symptoms including areas of dry, itching and reddened skin. Very often it is inherited; if you have one parent with the disease you have a greater than 50 per cent chance of developing it yourself.
The most common complaint we receive is about how itchy people’s skin gets. It’s a constant aggravation, leading to distraction during the day and disturbed sleep at night. And to make matters worse, scratching will generally cause the problem to flare up, leading to more itch. It’s a very unpleasant cycle.
2. What are the main causes of eczema?
Luke: The specific cause of eczema remains unknown, but it is believed to develop due to a complex combination of hereditary and environmental factors. While eczema is not contagious, children are more likely to develop eczema if a parent (or worse, parents) has had it or another atopic disease (like asthma or hayfever). These diseases are all examples of an immune system that has become hypersensitive. These diseases occur when the immune system decides that something relatively harmless is actually a danger to your health (think pollen and hayfever).
Environmental factors are also known to trigger (or worsen) episodes of eczema. These include:
- Irritants: soaps, detergents, shampoos, disinfectants, juices from fresh fruits, meats or vegetables
- Allergens: dust mites, pets, pollens, mold,
- Microbes: bacteria such as Staphylococcus aureus (Golden staph), viruses, certain fungi
- Hot and cold temperatures: hot weather, high and low humidity, perspiration from exercise
- Foods: dairy products, eggs, nuts and seeds, soy products, wheat
- Stress: both acute (e.g. bereavement) and chronic stress, as well as fatigue and anxiety
- Hormones: women can experience worsening of eczema symptoms at times when their hormone levels are changing, for example during pregnancy and at certain points in their menstrual cycle.
These are the most common triggers we see but it’s always worth keeping in mind that everybody is different, I’ve never seen two cases that were the same. Treatment always has to focus on treating symptoms as well as identifying an individual’s unique triggers to prevent further flare-ups.
3. Why is eczema becoming more common in children in particular?
Luke: There are a variety of theories, but one of the more convincing ones is the “Hygiene Hypothesis” which was first suggested in 1989 by David Strachan, an American immunologist. He argued that the decreased exposure to infections and the resulting cleaner environment in Western societies over the past decades has led to higher rates of atopic diseases in the population. The irony here is that the charge to prevent diseases caused by unsanitary conditions (think deadly diseases like cholera, typhoid etc.) may have accidentally led to an increase in hypersensitive immune conditions.
The Hygiene Hypothesis was originally based on the observation that the youngest child in a family has a lower risk of atopic diseases, particularly hay fever and eczema, compared with his or her older brothers and sisters. This was thought to be caused by the youngest child’s exposure to a wider range of infectious agents as their immune system developed, allowing their immune system to develop robust, appropriate (i.e. not overreacting to harmless triggers like dust etc.) responses to various challenges. Other observations seem to lend weight to this theory. For example, children growing up in a traditional farming environment and who have been exposed to a wider variety of bacteria, viruses and fungi have also shown lower rates of atopic diseases.
Another aspect of the Hygiene Hypothesis focuses more on the diversity of bacteria in a baby’s gut. Studies with infantile eczema have shown that certain probiotics can be useful in treating their eczema and it has also been noted that babies born via caesarean section have higher rates of eczema. This last fact is probably because natural birthing exposing babies to their mother’s bacterial makeup, essentially inoculating them at birth and beginning the immune system’s learning process.
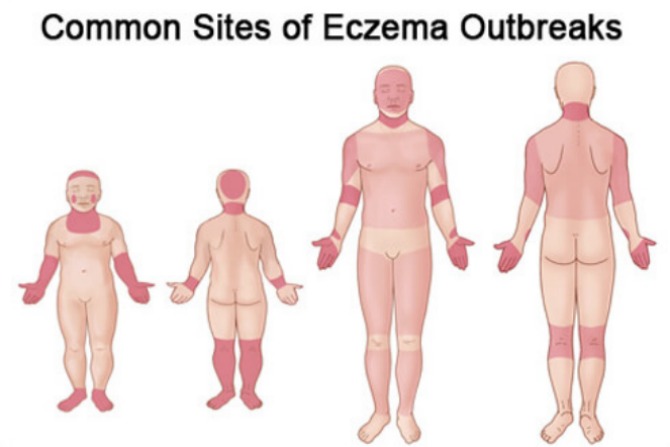
4. In what areas of the body does eczema usually appear?
Luke: So called “sites of predilection” change over the course of a person’s life but the diagram below shows the most common ones. However, in more severe cases it can be widespread or almost totally covering the skin.
5. Can a child suffering eczema still do things such as go swimming? Are there any activities in particular that can aggravate it?
Luke: In Canberra we have a problem: we don’t have any salt-water pools, which are generally better for sensitive skin. Chlorinated pools can be very irritating to eczema and some children should definitely avoid swimming when the condition is flaring. That said, adequate exercise is, of course, very important for children, so we need to make sure they are active.
However, because heat and sweat can be very irritating, sufferers are caught in a Catch-22; exercise would help them stay fit and healthy generally (and therefore positively affect their eczema) but the activity itself can flare up the skin!
As always, there are very few “one-size-fits-all” solutions to treating eczema in children, we need to adapt our approach on a case by case basis.
6. What are the treatment options?
Luke: In most cases, we start with moisturisers and work our way up from there. At our clinic we put great emphasis on dealing with triggers of the disease, including dietary, environmental (weather etc.) and psychological triggers (particularly stress). We also use ointments and creams to treat the symptoms but these are regarded as short-term solutions to relieve the maddening itchiness, as well as heal scratches and infected lesions, while we treat the underlying problem. And all of our products are steroid-free.
When a treatment focuses on addressing all the contributing factors that can cause or flare up eczema it has a much greater chance of delivering a long-term result. Our patients also gain a clearer understanding of the nature of their problem, so as to better manage their disease into the future.
If problems persist, contact Healthy Skin Solutions for a consultation on 6295 6040 or visit their website at healthyskinsolutions.com.au
ABOUT LUKE
Luke Clews originally trained as a Radiation Oncology Medical Physicist, before changing his career path to train under Dr Michael Tirant, a world-renowned pioneer of Complementary Dermatology. He now runs the Healthy Skin Solutions clinic in Kingston, treating a wide variety of common (and uncommon) skin problems including eczema, dermatitis, acne, rosacea, psoriasis and many more.
This is a sponsored post but all opinions are the author’s own. Find more information about our sponsored post policy here.



Leave a Reply